White Papers
The Rural Hospital Crisis


Rural hospitals face an existential threat as chronic staffing shortages intersect with mounting financial instability and pressure. This white paper examines the crisis, Medicaid’s role in rural hospital viability, the financial impact of proposed cuts, and survival strategies for healthcare and staffing stakeholders to consider.
The Rural Hospital Closure Crisis

Rural hospitals are an integral part of the American health system, ensuring that people in even the most isolated parts of the country have access to vital care. Research shows that one in seven Americans rely on rural hospitals for their health and the well-being of their communities[1]. Despite their importance, these facilities face a growing crisis fueled by financial challenges that has resulted in widespread closures across the country’s already underserved rural areas.
The scale of this crisis is staggering. The Center for Healthcare Quality and Payment Reform reports that over 100 rural hospitals have closed since 2015[2], while data from The Kaiser Family Foundation reveals there was a net reduction of 50 rural hospitals nationwide from 2017 to 2023. In contrast, urban areas saw a net reduction of 13 hospitals[3].
These closures stem from unique challenges facing rural hospitals. Serving smaller populations with smaller facilities results in lower patient volumes, difficulty providing specialized services, and greater vulnerability to economic fluctuations[4]. This combination leads to lower revenue and diminished economies of scale. Geographic isolation compounds these issues, as rural hospitals face greater expenses for medical equipment, supplies, and transportation.
The financial outlook is particularly dire. The data from the Center for Healthcare Quality and Payment Reform also reveals that nearly one-third of the country’s rural hospitals are at risk of closure due to financial instability, while more than 300 face “immediate risk” because they have suffered multiyear financial losses or maintain very low financial reserves[5].
In 2023 alone, 48% of rural hospitals operated at a financial loss[6].
Medicaid’s Role in Rural Hospital Viability

Given the financial pressures facing rural hospitals, Medicaid serves as a critical lifeline for these facilities and their communities. The program covers over 16 million people in rural areas, accounting for nearly 50% of all children and 18% of all adults in these communities[1].
Beyond providing coverage, Medicaid makes care more accessible, with research showing that both children and adults covered by Medicaid are more likely to have regular sources of care and receive preventive services[1]. Importantly, the program is vital in helping hospitals sustain operations, as higher rates of Medicaid coverage for adults correlate with improved hospital financial performance and lower likelihood of closure, particularly in areas that have expanded Medicaid[1].
The data on Medicaid expansion underscores its crucial role. Research indicates that the majority (74%) of rural hospital closures occurred in states where Medicaid expansion was not in place or had been in place for less than a year[10]. This pattern reflects the financial impact of reduced coverage, as operating margins are demonstrably lower in non expansion states. Conversely, hospitals in expansion states experienced almost 5% less uncompensated care costs[11].
However, this heavy reliance on Medicaid presents challenges. Studies indicate that Medicaid provides substantially lower reimbursement levels for physician services compared to Medicare and private insurance[12]. This payment gap further strains the already razor-thin margins on which rural hospitals operate, with many depending heavily on supplemental payments and provider taxes for survival.
Notably, rural critical access hospitals have access to cost-based reimbursement through Medicaid, which can partially offset higher labor costs. Because these facilities receive a higher proportion of Medicaid funding and maintain their critical access designation, they can receive reimbursement for travel nursing and contingent staffing at higher rates than their urban counterparts. This means that while a rural critical access hospital might pay $100 per hour for a traveler, they can recover a substantial portion of that cost through Medicaid reimbursement. This can make it less burdensome than an urban hospital paying $85 per hour without the same reimbursement structure.
However, reimbursement timelines can extend up to 12 months, creating significant cash flow challenges. This highlights the importance of hospitals maximizing their reimbursements through proper coding and ensuring they capture all eligible funding. In response to these challenges, many states have implemented special Medicaid payment rules to help rural hospitals secure higher reimbursement rates[3].
Financial Impact of Medicaid Cuts

Following the passage of the One Big Beautiful Bill Act (P.L. 119-21), rural hospitals may now face
even greater financial challenges stemming from enacted Medicaid changes.
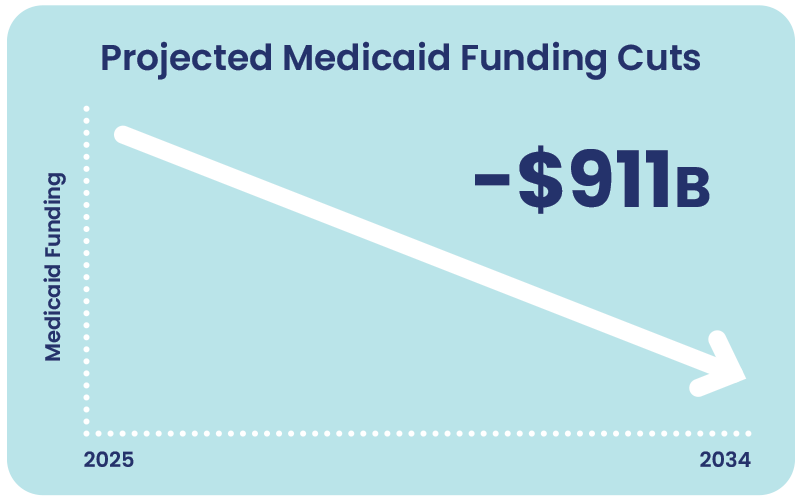
The Congressional Budget Office estimates the legislation will reduce federal Medicaid spending by approximately $911 billion over the next 10 years and result in 10 million people losing Medicaid coverage nationwide by 2034[13]. This impact is projected to be felt the most in states where Medicaid was not expanded.
It is important to note that the One Big Beautiful Bill Act and the Rural Health Transformation Program are two separate initiatives with distinct impacts. The One Big Beautiful Bill Act is projected to cut approximately $911 billion from Medicaid spending overall.
Subsequently, the Rural Health Transformation Program was established to put $50 billion back into the system, specifically designated for rural hospitals. This creates a net reduction of approximately $861 billion across federal Medicaid spending.
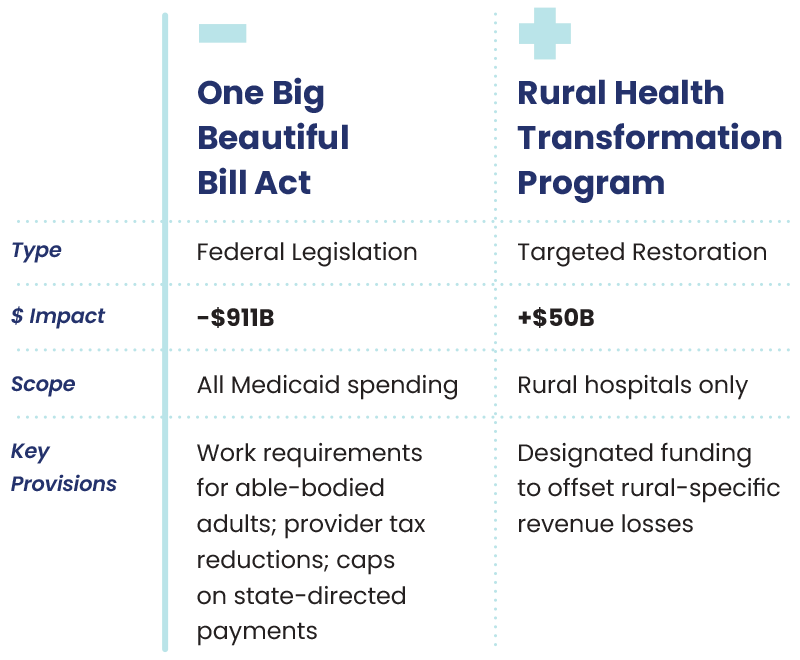
However, the ultimate impact on rural hospitals specifically remains uncertain. While they receive targeted funding through the transformation program, it is unclear whether rural facilities will come out ahead or behind when weighing the approximately $911 billion in overall Medicaid cuts against the $50 billion in rural-specific restoration.
The enacted provisions target multiple critical funding streams simultaneously. New work requirements for able-bodied adults, provider tax reductions, and caps on state-directed payments are now directly impacting rural hospital revenue. As a result, facilities may be forced to absorb substantially higher rates of uncompensated care at a time when margins are already negative for nearly half of all rural hospitals. Due to the dependence on Medicaid reimbursements, these payment reductions can ultimately force facilities into having to make difficult choices between maintaining services, keeping staff, or potentially closing.

Beyond healthcare delivery, there are also financial impacts to communities where rural hospitals close. This is because rural hospitals typically are the largest or second largest employer in their communities[14]. As hospitals struggle with reduced revenues, communities may feel wider ripple effects like workforce reductions, decreased local spending, and concerns about accelerating population loss.
Strategic Financial Survival Tactics

While the challenges are formidable, rural hospitals may want to consider implementing strategic approaches to improve financial resilience. Consider adopting a multi-faceted strategy that includes:
Revenue Cycle Management Optimization
With the high number of rural hospitals currently operating at a loss, healthcare finance experts recommend prioritizing revenue cycle management improvements as a potential pathway to sustainability[15].

Strategic Pricing Analysis
Hospitals may benefit from analyzing peer fee schedules and assessing local market sensitivities to identify revenue optimization opportunities. Advanced software tools can simulate previous year activities and provide tailored recommendations, potentially helping facilities capitalize on higher outpatient commercial reimbursement while remaining competitive.
Enhanced Charge Capture
Establishing more robust processes for documenting and billing all services rendered could help identify previously unbilled services and address billing discrepancies. Training video libraries and ongoing education programs may provide sustainable foundations for continuous improvement.
Outsourced Revenue Cycle Services
Some hospitals may find that partnering with outsourced revenue cycle management providers can help streamline billing processes, reduce administrative overhead, and improve cash flow while ensuring more timely reimbursements.
Strategic Workforce Management
Staffing shortages represent one of the most pressing challenges for rural hospitals because they can drive up costs while compromising service delivery. To help with this, it may be beneficial for hospitals to explore flexible staffing solutions that they traditionally may not have considered.

Healthcare Staffing Agency Partnerships
Working with reputable healthcare staffing agencies can provide rural hospitals with access to qualified professionals during peak demand periods, unexpected absences, or while recruiting permanent staff. This approach may help facilities maintain essential services without the long-term commitment and overhead costs associated with permanent hires
Managed Service Provider (MSP) Programs
Some hospitals may find value in partnering with MSP vendors who can centrally manage their contingent workforce needs. MSPs may help streamline the process of engaging multiple staffing agencies, potentially improving fill rates, standardizing rates, and providing better visibility into workforce spending. This consolidated approach could also reduce administrative burden while optimizing staffing costs.
Flexible Workforce Models
Consider implementing a balanced workforce strategy that combines permanent staff with flexible staffing solutions. This hybrid approach may allow hospitals to maintain core capabilities while adapting to fluctuating patient volumes and seasonal demands without overextending fixed labor costs.
It is worth noting that a common pitfall in workforce cost management is the instinct to cut bill rates for temporary and contract staff as a primary cost-reduction strategy. While this approach may seem financially wise, it typically reduces the quality and availability of temporary clinical staff, which in turn can lead to unfilled shifts, increased patient risk, and greater operational strain.
The most effective pathway to reducing contingent labor costs is often not lower rates, but lower usage. By partnering with the right strategic workforce partner, rural hospitals can explore how to develop a more stable workforce that reduces reliance on temporary staff and achieves sustainable cost reductions without compromising care quality.

Service Line Expansion Opportunities
Rural hospitals looking to improve financial performance may want to explore strategic service expansions and operational efficiencies. Key challenges that other hospitals have addressed include patient outmigration to urban centers, limited service offerings, and underutilized facilities[16].

Specialty Service Integration
Adding high-demand specialty services can capture revenue that would flow to urban facilities. To reduce upfront costs and operational risks for this approach, try partnering with specialty providers.
Operating Room Utilization
If your ORs are underutilized, try optimizing schedules or implementing specialty surgery days to help reduce idle time. This can also help generate additional revenue from existing infrastructure.
Community Engagement Initiatives
Expanding local services or planting relationship roots in your community can help with reducing patient outmigration and building referral networks of local physicians.
Strategic Partnerships and Collaboration
Financial survival in today’s environment may also increasingly depend on collaboration rather than isolation. Over the past few years, momentum has grown among rural hospitals to organize collectively and consolidate their spending, particularly around their highest cost categories, temporary labor expenditures. While hospital associations have traditionally focused on legislative advocacy and lobbying efforts, forward-thinking rural hospitals are now exploring how to leverage collective purchasing power and shared resources to improve access to talent while containing costs.
The state of Washington provides a notable example of this movement, where rural hospitals came together to create an organized approach that functions similarly to an internal MSP. While this model has shown promising results and represents the most comprehensive state-level initiative to date, the implementation proved more complex than initially anticipated. Most states are unlikely to replicate Washington’s full approach, but the underlying principles of collaboration and resource pooling remain valuable. Rural hospitals may benefit from considering the following partnership strategies

Network Development
Even independent hospitals might benefit from thinking in terms of networks, including referral relationships, shared services, and aligned contracting arrangements. Such networks could potentially improve staff recruitment and enable more efficient resource sharing.
Association Engagement and Best Practice Sharing
Hospitals should actively participate in association conferences and networking opportunities to share ideas and learn from peers who have successfully implemented collaborative approaches. These connections can provide valuable insights into staffing strategies, preferred vendor relationships, and group purchasing arrangements that have proven effective for other rural facilities.
Core Competency Focus
This would involve hospitals focusing resources on services they perform well and are strategically important, while exploring partnerships for areas where they face challenges. Building alliances or joint ventures could help maintain continuity of care and stabilize contracts.
Technology Integration
Hospitals may want to explore how AI and automation for routine operations could help relieve labor strain and improve operational efficiency. Modern financial management tools might also assist with forecasting future needs and streamlining budgeting processes.
Federal Funding and Grant Opportunities
Another beneficial approach for rural hospitals is actively pursuing federal funding opportunities and state grants that help maintain financial stability. Potential funding sources to investigate include

Rural Emergency Hospital (REH) Designation
This newer Medicare provider program offers monthly facility payments to eligible hospitals. Facilities considering this option should carefully evaluate whether the REH model aligns with their community’s needs and their long-term strategic goals.
USDA Community Facilities Program
Rural hospitals may find a higher chance of survival by pursuing Community Facilities Program funding. These grants and loans are designed to support essential community facilities for eligible rural hospitals
Rural Health Transformation Program
Separate from the One Big Beautiful Bill Act’s Medicaid cuts, this program establishes a $50 billion fund ($10 billion annually from 2026-2030) specifically for state rural health transformation plans [17]. All 50 states submitted applications, and awards were announced in December 2025. States are now receiving funding based on their rural hospital populations and specific needs, with awards distributed over five years.
Hospitals should work with state officials to understand their state’s approved plan and identify opportunities to benefit from these resources. Given the complexity and substantial commitment required, hospitals should approach engagement with this program strategically while recognizing its potential value for workforce development and operational improvements.
Looking Ahead

The rural hospital crisis represents both an urgent threat and an opportunity for transformative
change. With hundreds of rural hospitals at immediate risk and Medicaid cuts threatening billions of dollars in rural healthcare funding, the stakes could not be higher.
The path forward for rural hospitals will demand collaboration between rural hospital leaders, staffing professionals, policymakers, and rural health advocates. By implementing strategic financial survival tactics while pursuing necessary policy aid, rural hospital stakeholders can work together to ensure that their communities continue to have access to quality healthcare services.
The path forward for rural hospitals will demand collaboration between rural hospital leaders, staffing professionals, policymakers, and rural health advocates
References
- American Hospital Association. (2025, June 5). Medicaid coverage supports rural patients, hospitals, and
communities. https://www.aha.org/fact-sheets/2025-06-05-medicaid-coverage-supports-rural-patientshospitals-
and-communities - Center for Healthcare Quality and Payment Reform. (2025, October). Problems and solutions for rural hospitals.
Saving Rural Hospitals; Center for Healthcare Quality and Payment Reform. https://ruralhospitals.chqpr.org/
Overview.html - Kaiser Family Foundation. (n.d.). Key facts about hospitals. https://www.kff.org/key-facts-about-hospitals/
- Levinson, Z., Godwin, J., & Hulver, S. (2023, February 23). Rural hospitals face renewed financial challenges,
especially in states that have not expanded Medicaid. Kaiser Family Foundation. https://www.kff.org/health-costs/
issue-brief/rural-hospitals-face-renewed-financial-challenges-especially-in-states-that-have-not-expandedmedicaid/ - Center for Healthcare Quality and Payment Reform. (n.d.). Rural hospitals at risk of closing. (2025). Center for
Healthcare Quality and Payment Reform. https://chqpr.org/downloads/Rural_Hospitals_at_Risk_of_Closing.pdf - American Hospital Association. (2025, June 13). Rural hospitals at risk: Cuts to Medicaid would further threaten
access. https://www.aha.org/fact-sheets/2025-06-13-rural-hospitals-risk-cuts-medicaid-would-furtherthreaten-
access - U.S. Government Accountability Office. (2021). Rural hospital closures: Affected residents had reduced access to
health care services (GAO-21-93). https://www.gao.gov/products/gao-21-93 - Gujral, K., & Basu, A. (2019, August 1). Impact of rural and urban hospital closures on inpatient mortality. National
Bureau of Economic Research. https://www.nber.org/papers/w26182 - Durrance, C., Guldi, M., & Schulkind, L. (2023). The effect of rural hospital closures on maternal and infant health.
Health Services Research, 59(2). https://doi.org/10.1111/1475-6773.14248 - American Hospital Association. (2022). Rural hospital closures threaten access solutions to preserve care in local
communities. https://www.aha.org/system/files/media/file/2022/09/rural-hospital-closures-threaten-accessreport.
pdf - National Rural Health Association. (2025, April). Critical condition: How Medicaid cuts would reshape rural health
care landscapes. https://www.ruralhealth.us/blogs/2025/04/critical-condition-how-medicaid-cuts-wouldreshape-
rural-health-care-landscapes - Callison, K., & Nguyen, B. T. (2017). The effect of Medicaid physician fee increases on health care access, utilization,
and expenditures. Health Services Research, 53(2), 690–710. https://doi.org/10.1111/1475-6773.12698 - National Rural Health Association. (2025). Estimated impact on Medicaid enrollment and hospital expenditures in
rural communities. In National Rural Health Association. National Rural Health Association. https://www.ruralhealth.
us/nationalruralhealth/media/documents/advocacy/2025/obbb-impacts-on-rural-communities_06-20-25-
final_v3-(002).pdf - Ricketts, T. C., 3rd, & Heaphy, P. E. (2000). Hospitals in rural America. The Western journal of medicine, 173(6),
418–422. https://doi.org/10.1136/ewjm.173.6.418 - National Rural Health Association. (2025, April). Hidden dollars: A rural hospital’s guide to financial survival. https://
www.ruralhealth.us/blogs/2025/04/hidden-dollars-a-rural-hospital%E2%80%99s-guide-to-financial-survival - National Rural Health Association. (2025, February). Overcoming barriers to sustainable growth in rural hospitals.
https://www.ruralhealth.us/blogs/2025/02/overcoming-barriers-to-sustainable-growth-in-rural-hospitals - Kaiser Family Foundation. (2025, August 4). A closer look at the $50 billion rural health fund in the new
reconciliation law. https://www.kff.org/medicaid/a-closer-look-at-the-50-billion-rural-health-fund-in-the-newreconciliation-
law/
Do you need help quickly finding qualified healthcare professionals for your facility?
Get the latest blogs, news and company updates
Want to get the latest staffing related news and updates? Subscribe to our resources to get insights sent straight to your inbox.